TL;DR:
Semaglutide, a groundbreaking semaglutide obesity medication, offers a dual benefit in managing weight and treating type 2 diabetes. Working like a natural appetite hormone, it reduces food intake, improves metabolism, and promotes feelings of fullness. Clinical trials show significant weight loss and positive health markers with once-weekly administration, making it a convenient addition to multidisciplinary treatment plans.
Effective for individuals with BMIs ranging from 30-40 kg/m² or above 27 kg/m² with comorbidities, semaglutide should be personalized based on patient needs and adherence. While side effects like nausea may occur, proper management through dietary adjustments and dosage monitoring ensures a safer experience. Combining semaglutide with tailored lifestyle interventions proves highly effective for weight loss and metabolic health improvement. Future research aims to explore its long-term efficacy, safety, and potential in preventing weight regain.
“Obesity is a complex, multifaceted health challenge, demanding a comprehensive approach. In this article, we explore Semaglutide as a powerful tool in the fight against obesity. As a novel semaglutide obesity medication, it offers promising solutions for weight management. We delve into its mechanism of action, uncovering how it suppresses appetite and regulates insulin. Beyond its benefits, we discuss integrating semaglutide into a multidisciplinary treatment plan, emphasizing patient selection and lifestyle interventions. By combining medical expertise with personalized care, this article aims to provide insights into harnessing the potential of semaglutide for lasting weight loss.”
Understanding Obesity and Its Complexities
Obesity is a multifaceted health condition characterized by excessive fat accumulation that impairs overall well-being and increases the risk of various chronic diseases. It’s more than just weight; it’s influenced by genetic, environmental, psychological, and behavioral factors. The complexity lies in the fact that these factors interact, creating a web of challenges that contribute to obesity’s prevalence as a global health concern.
Semaglutide, an innovative semaglutide obesity medication, emerges as a promising tool in navigating this complex landscape. As part of a multidisciplinary approach to treating obesity, semaglutide can help address the underlying hormonal and physiological mechanisms contributing to weight gain. Its effectiveness lies not only in its ability to suppress appetite but also in its potential to induce long-term lifestyle changes, thereby offering a sustainable solution for managing obesity and mitigating associated health risks.
The Role of Semaglutide in Weight Management

Semaglutide, a relatively new obesity medication, plays a pivotal role in comprehensive weight management strategies. As a glucagon-like peptide-1 (GLP-1) receptor agonist, it mimics the natural hormone GLP-1, which is secreted after eating. This action promotes feelings of fullness and reduces appetite, leading to decreased calorie intake. In clinical trials, semaglutide has demonstrated significant weight loss effects when administered as part of a multidisciplinary approach.
This medication not only aids in weight reduction but also improves various metabolic markers associated with obesity, such as blood pressure, cholesterol levels, and blood sugar control. Its long-acting formulation allows for once-weekly administration, providing convenience and consistency in adherence to treatment plans. Additionally, semaglutide has shown promising results in maintaining lost weight over time, making it a valuable tool in the ongoing battle against obesity.
Mechanism of Action: How Semaglutide Works
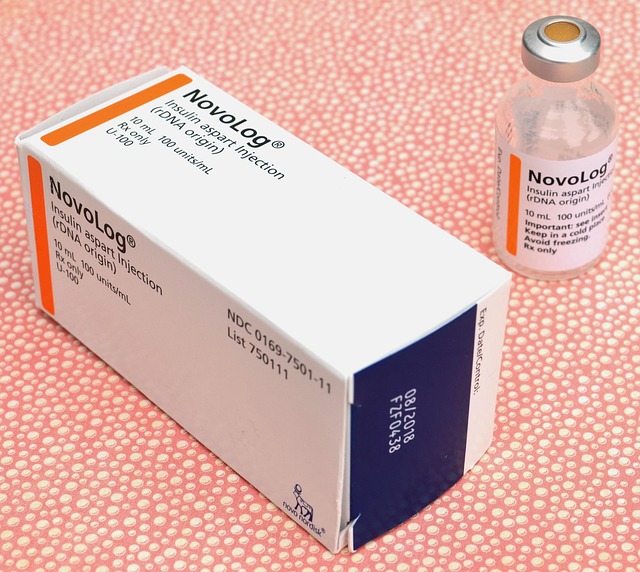
Semaglutide, an innovative obesity medication, has gained significant attention for its dual role in weight management and type 2 diabetes treatment. Its mechanism of action involves mimicking the effects of natural hormones, leading to profound effects on hunger and satiety. By activating specific receptors in the brain, semaglutide suppresses appetite, resulting in reduced food intake and subsequent weight loss.
This medication stimulates the release of peptides that promote feelings of fullness, while also slowing gastric emptying. This dual action not only helps individuals eat less but also improves insulin secretion and glucose control, making it a valuable tool in the multidisciplinary approach to obesity treatment.
Benefits of Semaglutide as a Medication

Semaglutide, an innovative obesity medication, has gained significant attention in recent years due to its multifaceted benefits. It works by mimicking a natural hormone that regulates appetite and glucose levels, leading to reduced food intake and improved metabolism. This dual action not only aids in weight loss but also helps manage type 2 diabetes, making it a game-changer for many individuals struggling with these conditions simultaneously.
As a semaglutide obesity medication, it offers a unique approach compared to traditional dietary and exercise interventions alone. Studies show that semaglutide can help patients lose significant amounts of weight, often leading to improvements in overall health markers such as blood pressure and cholesterol levels. Additionally, its long-acting formulation allows for once-weekly administration, simplifying treatment adherence and enhancing patient convenience.
Integrating Semaglutide into a Multidisciplinary Approach

Integrating Semaglutide into a Multidisciplinary Approach offers a comprehensive solution for managing obesity. As a powerful semaglutide obesity medication, it plays a pivotal role in this strategy by addressing physiological aspects of weight regulation. This injectable medication works by mimicking natural hormones to curb appetite and slow gastric emptying, leading to reduced calorie intake and increased feelings of fullness.
This treatment is most effective when combined with other components like dietary counseling, exercise programs, and behavioral interventions. These complementary methods target the psychological and social facets of obesity, ensuring a holistic approach. By integrating semaglutide into this multidisciplinary framework, healthcare providers can offer personalized care that not only aids in weight loss but also fosters long-term lifestyle modifications for sustained health improvements.
Patient Selection and Individualized Treatment Plans

Patient selection is a critical aspect when incorporating semaglutide, a powerful semaglutide obesity medication, into a multidisciplinary approach to treat obesity. This therapy is most suitable for individuals with a body mass index (BMI) typically between 30 kg/m² and 40 kg/m² or those with BMI over 27 kg/m² with comorbidities. The decision should also consider the patient’s motivation, lifestyle, and willingness to commit to the treatment plan.
Individualized treatment plans are essential as semaglutide is a personalized medicine. Healthcare professionals must carefully evaluate each patient’s unique needs, preferences, and health history. This may include adjusting dosage or even combining semaglutide with other obesity treatments like behavioral therapy, diet planning, and exercise programs to achieve optimal results and improve patient adherence.
Potential Side Effects and Management Strategies
Semaglutide, as an innovative obesity medication, offers a promising path to weight management. However, like any treatment, it’s not without potential side effects. Common experiences include nausea, vomiting, diarrhea, and constipation – often early in the treatment journey. These can be managed through dietary adjustments, increasing fluid intake, and adhering to prescribed doses.
For more severe reactions, medical professionals may recommend monitoring strategies. Regular check-ins with healthcare providers allow for close observation of both weight loss progress and any adverse effects. Adjustments to dosage or treatment plans can be made as needed, ensuring a safer and more effective semaglutide obesity medication experience tailored to individual needs.
Combining Semaglutide with Lifestyle Interventions

Combining semaglutide with lifestyle interventions offers a comprehensive approach to managing obesity, enhancing its effectiveness as a semi-synthetic glucose-dependent insulinotropic polypeptide (GIP) analog. This dual strategy leverages the medication’s ability to suppress appetite and regulate blood sugar, while lifestyle changes, such as improved nutrition and increased physical activity, further contribute to weight loss.
In clinical settings, integrating semaglutide into a multidisciplinary treatment plan has shown promising results. Lifestyle modifications, tailored to individual needs, complement the drug’s action by fostering healthier habits that sustain long-term weight management. Consequently, this synergistic effect not only aids in achieving significant weight loss but also improves overall metabolic health, making it a valuable tool in the fight against obesity.
Future Perspectives and Research Directions

As research in the field of obesity treatment continues to evolve, future perspectives for semaglutide as a part of multidisciplinary care look promising. Ongoing and upcoming clinical trials are expected to provide valuable insights into its long-term efficacy and safety, particularly when combined with behavioral interventions. These studies may explore optimal dosing strategies and identify patient subpopulations that could benefit most from this medication. Additionally, investigating the potential of semaglutide in preventing weight regain after initial weight loss is an exciting direction.
The integration of semaglutide into routine clinical practice requires further examination. Cost-effectiveness analyses and real-world studies can help determine its place in treatment algorithms alongside other obesity medications. Moreover, understanding patient preferences and adherence to semaglutide therapy is crucial for optimizing outcomes. Future research should also delve into the potential combination of semaglutide with other novel weight management interventions, such as behavioral technologies or personalized nutrition plans, to create comprehensive, tailored treatments for obesity.
